The Future of Robotic Surgery, Part 2
The field of surgical robotics continues to evolve at a rapid pace. Intuitive Surgical was the first company to market and currently dominates the field, but other large players such as Johnson & Johnson, Medtronic and Stryker are entering the space, along with a host of smaller medical device companies. In Part 2 of our series, we explore how advancements in sensor technologies, haptics, and usability / ergonomics are opening up new possibilities and applications for robotic surgery.

4. Sensor Technologies
Small, high precision sensors used for imaging, force, pressure, torque, and other measurement parameters can be critical to a surgical robot’s performance and potential applications. Manta client Medrobotics’ Flex Robotic System incorporates a high-resolution camera to provide surgeons 3D high-definition visualization of both the navigation path and surgical site. Vicarious Surgical is exploring the use of virtual reality headsets coupled with a high-resolution camera to provide surgeons the perspective of being inside the patient.
Vision sensors combined with touch sensors are being used to increase the adaptability and intelligence of the surgical robot. The STAR robot developed by Children’s National Health System in D.C. uses touch and vision sensors to locate valve leaks in the heart. To pinpoint its precise location, the robot makes repeated gentle tapping contact with the heart wall. In animal trials this year, the robot successfully navigated from its entry point to the damaged valve area 95% of the time.
And in the lab, researchers like those at MIT’s MCube Lab, which spun out Manta client Gelsight, are also developing vision-based tactile sensors. These sensors could be used to provide surgeons with high-resolution images of the texture and topography of tissue.

Surgeons will rely less on traditional direct visualization and tactile interaction as new sensor technologies provide enhanced 3D visualization.
5. Haptics
Haptics, also known as kinaesthetic communication or 3D touch, refers to the use of touch to communicate information to users. Haptics typically involves applying forces, vibrations, or motions to the user, such as the vibration of a cell phone or game controller. In surgical robotic applications, haptic feedback to the surgeon is typically linked to the outputs of sensors that are incorporated into the robot components that enter the patient.
Many current robotic-assisted surgical systems lack sufficient and accurate haptic feedback, which surgeons otherwise use to navigate, detect tissue, and gauge forces. A lack of such haptic feedback makes it difficult for a surgeon to maintain precise control without damaging surrounding tissues. Accordingly, various groups are beginning to embed force and other sensors into robotic arms. Haptic enabling sensors require both miniaturization and biocompatibility. In single use applications, these sensors also need to be highly cost-effective. In reusable applications, the sensors need to be autoclavable / re-sterilizable.
One of the most significant advances in haptics was made by Mako Surgical (acquired by Stryker for $1.65B). In 2006, the company began offering a robot that provides precise feedback to surgeons repairing arthritic knee joints. More recently, Cambridge Research & Development pioneered a new haptic device that a surgeon can wear anywhere on the body which uses linear actuation to mimic the sense of touch.
By coupling haptic feedback to force, pressure, torque and other sensors resident in the surgical robotic instruments, surgeons can obtain greater feedback that improves accuracy and dexterity while minimizing trauma to the patient.
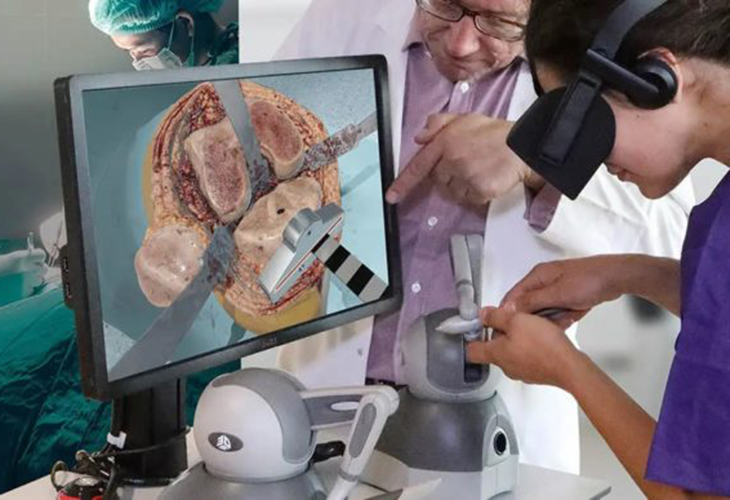
Haptic enabled robotic-assisted surgical systems greatly enhance the surgeon's ability to sense and "feel" anatomical features.
6. Usability and Ergonomics
Ergonomics and comfort are key drivers for surgeons’ adoption of robotic systems. The design of robotic surgery systems offers the potential for improvements over the ergonomics of traditional surgery by putting surgeons in a more upright position, such as with Intuitive’s console. Manta client Corindus’ Corepath GPX System offers the dual benefit of reduced radiation and elimating the requirement to wear heavy lead aprons during the procedure, as the control module is remotely located from the radiation path. These lead aprons are well documented to cause orthopedic problems in surgeons and other operating room personnel over time.
Even more critical is the design of the robotic controls, both in the type and layout of the controls. Controlling surgical robots typically involves two types of grips: the "pinch grip" and "power grip." The pinch grip, which brings together the thumb, middle, and index fingers, has been used in surgery for centuries to achieve high-precision movements. On the other hand, the power grip involves grabbing a handle with the entire hand and is more suitable for forceful work and large movements.
Because the pinch grip puts tension on certain muscles of the hand and fingers, it is more likely to cause finger fatigue and discomfort in the hand. This can negatively impact the overall performance of surgical procedures. Although the power grip does not seem to cause such discomfort, it offers less precise control. As Manta VP of Design Betsy Goodrich has observed as part of the development a wide variety of surgical instruments, an individual surgeon’s hand size and natural grip strength can also impact control and feelings of discomfort.
Now, new robotic surgery systems, like one designed at the Tokyo Institute of Technology, are finding ways to offer both types of grips, along with a combined grip that results in more efficient positioning and performance, ease of use, and greater comfort. Ergonomic assessments, like those done by MANTA UI / UX researchers and designers, can lead to improved designs that decrease muscular fatigue while preserving instrument performance.
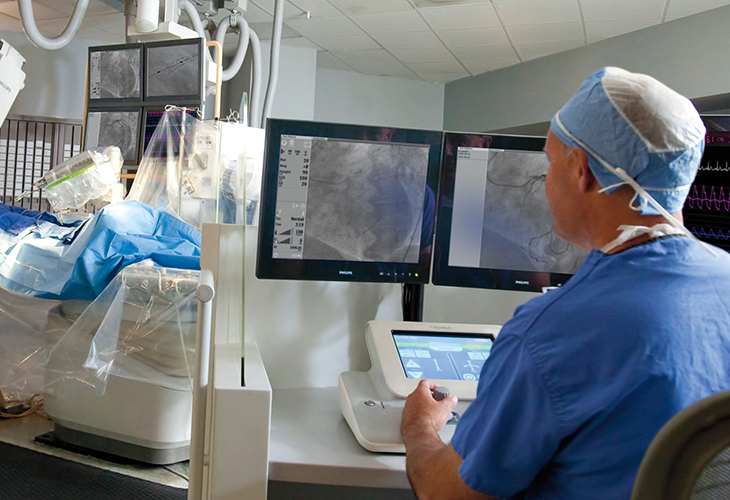
Robot-assisted surgical systems improve a surgeon's abilities and extend careers by eliminating awkward or stressful maneuvers and resulting in improved accuracy, sustained mental focus and reduced fatigue.
Conclusion: Impact of Robots on the Future of Surgical Procedures
Robotic surgery is evolving at a rapid pace both in terms of new technologies and applications. With the promise of enabling greater precision and more minimally invasive approaches, robotic surgery can lead to improvements in patient recovery and outcomes across the board.
Surgeon training remains an important item related to widespread implementation of robotic surgery. As robotic surgical systems become more autonomous, the hope is that they will reduce the training time for complex procedures. This would ideally increase the number of competent practicing surgeons.
Patient access is another factor that needs to be addressed. Access to surgery is unevenly distributed globally, but robotic arms and micro instruments that a surgeon can remotely control raises the prospects of telesurgery as a way to improve access to immediate, high-quality surgical care. As a test case, our client Corindus’ research in India demonstrated the world’s first percutaneous coronary intervention (PCI) conducted remotely outside the Cath lab.
Robotic surgery offers great promise, but is still very much an evolving field. The greatest challenge in the future of robotic surgery will be demonstrating the improvement these systems deliver on surgical performance and patient outcomes over traditional methods. To this end, sensor technologies, haptics and system ergonomics will all play critical roles.
MANTA
Our experienced team of researchers, designers, and engineers can help you create a standout user experience, elegant enclosures, and cutting-edge mechanical solutions for your robot - no matter the industry. Get started now.

when will generic cialis be available
when will generic cialis be available
zoloft interactions
zoloft interactions
metronidazole carbamazepine
metronidazole carbamazepine
can you take fluoxetine on an empty stomach
can you take fluoxetine on an empty stomach
cymbalta and weight gain
cymbalta and weight gain
does lexapro cause insomnia
does lexapro cause insomnia
fluoxetine or escitalopram
fluoxetine or escitalopram
gabapentin tagamet
gabapentin tagamet
buy generic viagra online europe
buy generic viagra online europe
bactrim vs keflex for skin infection
bactrim vs keflex for skin infection
cephalexin side effects for dogs
cephalexin side effects for dogs
accidentally took double dose of duloxetine
accidentally took double dose of duloxetine
other names for ciprofloxacin
other names for ciprofloxacin
para que sirve el cephalexin
para que sirve el cephalexin
bactrim bacteriostatic or bactericidal
bactrim bacteriostatic or bactericidal
bactrim ds tablet
bactrim ds tablet
price of neurontin walmart
price of neurontin walmart
amoxicillin 500mg capsules
amoxicillin 500mg capsules
diltiazem for afib dose
diltiazem for afib dose
can you take flexeril with ibuprofen
can you take flexeril with ibuprofen
sigla ddavp
sigla ddavp
flomax 700 a cosa serve
flomax 700 a cosa serve
simultaneous liquid chromatographic determination of ezetimibe and simvastatin in pharmaceutical products
simultaneous liquid chromatographic determination of ezetimibe and simvastatin in pharmaceutical products
side effects of effexor xr
side effects of effexor xr
depakote sexual side effects
depakote sexual side effects
cozaar recall 2018
cozaar recall 2018
can augmentin cause a yeast infection
can augmentin cause a yeast infection
diclofenac sodium 75mg dr tab
diclofenac sodium 75mg dr tab
not losing weight on contrave
not losing weight on contrave
what are the most common side effects of citalopram?
what are the most common side effects of citalopram?
aripiprazole cost walgreens
aripiprazole cost walgreens
dog aspirin dose
dog aspirin dose
allopurinol structure
allopurinol structure
amitriptyline dosage for pain
amitriptyline dosage for pain
buspar depression
buspar depression
how many mg of ashwagandha
how many mg of ashwagandha
augmentin with food
augmentin with food
celecoxib 100mg side effects
celecoxib 100mg side effects
does bupropion cause weight gain
does bupropion cause weight gain
is semaglutide available in new zealand
is semaglutide available in new zealand
acarbose contraindications
acarbose contraindications
what is the drug remeron used for
what is the drug remeron used for
protonix classification
protonix classification
how long does it take robaxin to work
how long does it take robaxin to work
snl abilify
snl abilify
actos advisor
actos advisor
repaglinide e scompenso cardiaco
repaglinide e scompenso cardiaco
ivermectin lotion for scabies
ivermectin lotion for scabies
tamsulosin bei nierenkolik
tamsulosin bei nierenkolik
voltaren gel price walgreens
voltaren gel price walgreens
synthroid antihistamines
synthroid antihistamines
empagliflozin vs sitagliptin
empagliflozin vs sitagliptin
venlafaxine 37.5 mg for migraines
venlafaxine 37.5 mg for migraines
spironolactone potassium sparing
spironolactone potassium sparing
is tizanidine a muscle relaxer
is tizanidine a muscle relaxer
accutane pharmacy coupons
accutane pharmacy coupons
cialis online pills
cialis online pills
sildenafil good rx
sildenafil good rx
sildenafil mechanism of action
sildenafil mechanism of action
online pharmacy same day delivery
online pharmacy same day delivery
tadalafil combitic
tadalafil combitic
levitra cost per pill at walmart
levitra cost per pill at walmart
levitra 10mg online
levitra 10mg online
can you buy stromectol over the counter
can you buy stromectol over the counter
tadalafil generic reviews
tadalafil generic reviews
viagra generic 20 mg
viagra generic 20 mg
price of ivermectin
price of ivermectin
ivermectin 8000
ivermectin 8000
viagra 100mg online buy
viagra 100mg online buy
stromectol how much it cost
stromectol how much it cost
slevotra vardenafil
slevotra vardenafil
stromectol medicine
stromectol medicine
vardenafil 20 mg price
vardenafil 20 mg price
generic tadalafil online
generic tadalafil online
ivermectin 3mg tablet
ivermectin 3mg tablet
trazodone for sleep reviews
trazodone for sleep reviews
is keflex safe in pregnancy
is keflex safe in pregnancy
ciprofloxacin over the counter
ciprofloxacin over the counter
how effective is valacyclovir
how effective is valacyclovir
tamoxifen nursing considerations
tamoxifen nursing considerations
augmentin sinus infection
augmentin sinus infection
low cost provigil
low cost provigil
how long does cephalexin take to work for uti
how long does cephalexin take to work for uti
amoxicillin for chlamydia
amoxicillin for chlamydia
can i take doxycycline 8 hours apart
can i take doxycycline 8 hours apart
can lisinopril be crushed
can lisinopril be crushed
how does lyrica make you feel
how does lyrica make you feel
metformin hair loss
metformin hair loss
order levitra online
order levitra online
testosterone gel online pharmacy
testosterone gel online pharmacy
viagra and cialis together
viagra and cialis together
tadalafil 5mg reviews
tadalafil 5mg reviews
vardenafil (levitra)
vardenafil (levitra)
can you buy sildenafil over the counter
can you buy sildenafil over the counter
sildenafil tablet
sildenafil tablet
sildenafil pills
sildenafil pills
sildenafil dose for high blood pressure
sildenafil dose for high blood pressure
sildenafil 25 mg tablet
sildenafil 25 mg tablet
tadalafil dosage 10 mg
tadalafil dosage 10 mg
what does viagra cost at a pharmacy
what does viagra cost at a pharmacy
how quickly does cialis work
how quickly does cialis work
order levitra tablets
order levitra tablets
buy generic levitra
buy generic levitra
sildenafil reddit
sildenafil reddit
what is the difference between sildenafil and tadalafil
what is the difference between sildenafil and tadalafil
online pharmacy to buy viagra
online pharmacy to buy viagra
buy levitra buy
buy levitra buy
buy levitra next day delivery
buy levitra next day delivery
mexico pharmacy codeine
mexico pharmacy codeine
sildenafil for pe
sildenafil for pe
cialis side effects heart
cialis side effects heart
what’s the difference between sildenafil and tadalafil
what’s the difference between sildenafil and tadalafil
levitra online pharmacy
levitra online pharmacy
vardenafil 20mg tablets
vardenafil 20mg tablets
precision pharmacy omeprazole powder
precision pharmacy omeprazole powder
tadalafil powder
tadalafil powder
vardenafil 20mg sublingual tablets
vardenafil 20mg sublingual tablets
tadalafil dosage for ed
tadalafil dosage for ed
spain pharmacy viagra
spain pharmacy viagra
global rx pharmacy irvine
global rx pharmacy irvine
usa pharmacy
usa pharmacy
can you cut a 20mg tadalafil in half
can you cut a 20mg tadalafil in half
online pharmacy india cialis
online pharmacy india cialis
priligy online pharmacy
priligy online pharmacy
does tadalafil make you last longer
does tadalafil make you last longer
tadalafil cost
tadalafil cost
how much ibuprofen for infant
how much ibuprofen for infant
does carbamazepine cause high blood pressure
does carbamazepine cause high blood pressure
can you give triaminic and motrin together
can you give triaminic and motrin together
arthritis medication celebrex
arthritis medication celebrex
sulfasalazine used for rheumatoid arthritis
sulfasalazine used for rheumatoid arthritis
gabapentin update
gabapentin update
celecoxib in prostate cancer treatment
celecoxib in prostate cancer treatment
etodolac 600 mg dosage
etodolac 600 mg dosage
gabapentin side effects for dogs
gabapentin side effects for dogs
que es la tegretol
que es la tegretol
diclofenac 75mg high
diclofenac 75mg high
can i take imitrex and oxycodone together
can i take imitrex and oxycodone together
reacciones adversas del cilostazol
reacciones adversas del cilostazol
indomethacin dosage in pregnancy
indomethacin dosage in pregnancy
amitriptyline nerve pain
amitriptyline nerve pain
can i order generic pyridostigmine online
can i order generic pyridostigmine online
bijwerkingen van mestinon
bijwerkingen van mestinon
how to pronounce mebeverine
how to pronounce mebeverine
elavil and blood pressure
elavil and blood pressure
imdur drug action
imdur drug action
can you stop taking baclofen
can you stop taking baclofen
obat wiros piroxicam
obat wiros piroxicam
sumatriptan-naproxen for acute treatment of migraine a randomized trial
sumatriptan-naproxen for acute treatment of migraine a randomized trial
does mobic have ibuprofen in it
does mobic have ibuprofen in it
maxalt no longer working
maxalt no longer working
lioresal sevrage alcoolique
lioresal sevrage alcoolique
quanto custa o meloxicam
quanto custa o meloxicam
azathioprine (imuran) is used for
azathioprine (imuran) is used for
frovatriptan e rizatriptan
frovatriptan e rizatriptan
azathioprine desensitization
azathioprine desensitization
periactin pediatric dosage
periactin pediatric dosage
dominos artane deals
dominos artane deals
how can i get ketorolac pills
how can i get ketorolac pills
cyproheptadine appetite dogs
cyproheptadine appetite dogs
how to get generic toradol pills
how to get generic toradol pills
zanaflex 4 mg tablets
zanaflex 4 mg tablets
hydrocodone tizanidine interaction
hydrocodone tizanidine interaction
sildenafil teva 5342
sildenafil teva 5342
viagra and indigestion
viagra and indigestion
cialis lowest price
cialis lowest price