The Future of Robotic Surgery, Part 1
Following our last deep-dive into medical robots, we're now turning to how advancements in surgical robotics are shaping the future of surgery. Though first successfully used in urology and gynecological procedures, robotic systems are penetrating a range of specialties, now most commonly used in thoracic and GI surgeries. In orthopedics, Medtronic’s acquisition of Mazor quickly catapulted it into market leadership, trailing only Intuitive and Johnson & Johnson.
For surgeons, the benefits of these systems include a smaller incision, better control, precision, and access to hard-to-reach areas. However, the field is still developing in both technology and adoption, especially with surgeons unhappy with excess physical strain and lack of tactile feedback. Advances in sensor technology and artificial intelligence are improving the precision, grip, feedback, and autonomy of robotic surgery systems.
Emerging robotics companies, like Microbot Medical, maker of a single-use robotic system, are harnessing these technologies to address market needs while challenging the capital-intensive models of established players. Investors are also sensing the opportunity; funding for robotics surgery companies, like Vicarious Surgical, drove record-setting healthcare investments in 2020.
The future of robotic surgery is moving towards more usable, intelligent robotic systems that can perform a greater range of procedures. In part one of this series, we explore how advancements in imaging, machine learning, and robotic end-effectors are enabling robotics companies to better deliver on the early promises of robots in the OR.

1. Augmented Visualization and Guidance
Image-guided navigation, which can incorporate imaging from CT scans, ultrasounds, or fluoroscopy, is becoming standard in robotic platforms because it provides direct vision to otherwise obscured anatomy. Surgeries that were once impossible because of the target location in the body are now feasible. Navigation is particularly helpful during minimally invasive procedures, which restrict the surgeon’s vision of the operating area.
In Medtronic’s Mazor platform, for instance, 3D cameras map the surgical site for optimal robotic arm movement, which reportedly increases accuracy. Robotic cameras can also emit and quantify tissue autofluorescence of reflectance spectra to highlight any microscopic surgical pathology for resection.
Multi-modal visualization, where 3D anatomical models are overlayed on live video feeds, represents the cutting-edge of surgical navigation systems, especially for robotic platforms. This type of visualization, also considered augmented reality for surgery, visualizes lesions or structures that a surgeon would otherwise only sense by touch. In laparoscopies, AR-techniques have been shown to reduce surgeons’ cognitive load, thereby improving efficiency. However, current solutions require improved depth perception and more sophisticated tracking to better detect instruments in the body.
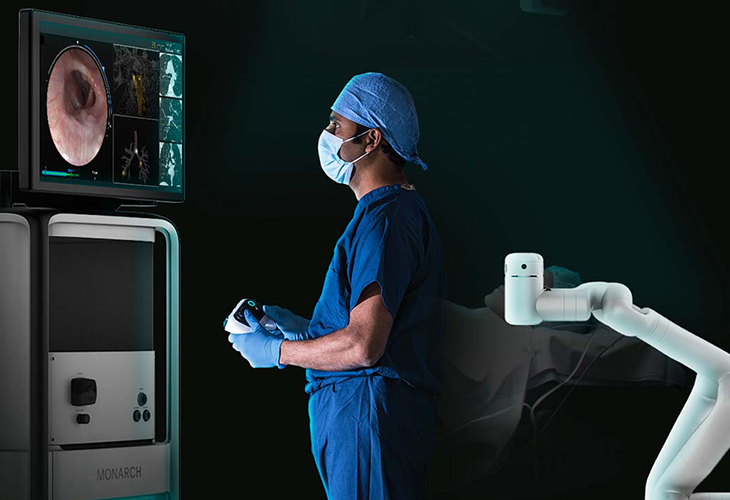
Johnson and Johnson's Monarch platform enables physicians to navigate the flexible robotic endoscope through the lung using a handheld controller and image-guidance.
2. Greater Autonomy
Developments in sensor technology have also fueled advances in complementing technology - artificial intelligence (AI). Some systems, such as the Titan Sport, harness automation to position cameras by tracking the surgeon’s gaze or the position of their instruments.
Others, like the Accuray Cyberknife S7, which launched last year, are fully autonomous. The Cyberknife S7 uses AI to adapt radiation delivery in real-time to patient. This precision improves workflow efficiency and benefits the patient by drastically reducing the days of radiation treatment and the chance of off-target hazards. Likewise in knee replacements, autonomous robots can cut through bone with greater accuracy than human surgeons.
For a robot to achieve such accuracy while autonomously manipulating soft tissue, however, is more difficult. Semi-autonomous suturing is a ‘grand challenge’ problem of surgical robotics. The STAR robot, an entirely autonomous system, includes a custom force-sensitive device for suturing soft tissue and a near-infrared camera that captures soft tissue injected with fluorescent markers.
Intelligent surgical robots with varying degrees of autonomy are proving in early tests to be the equals of surgeons at some technical tasks, such as locating wounds, suturing and removing tumors. That next level of assistance allows surgeons to perform intricate surgical feats without worrying that their hands might slip or their grip falter.
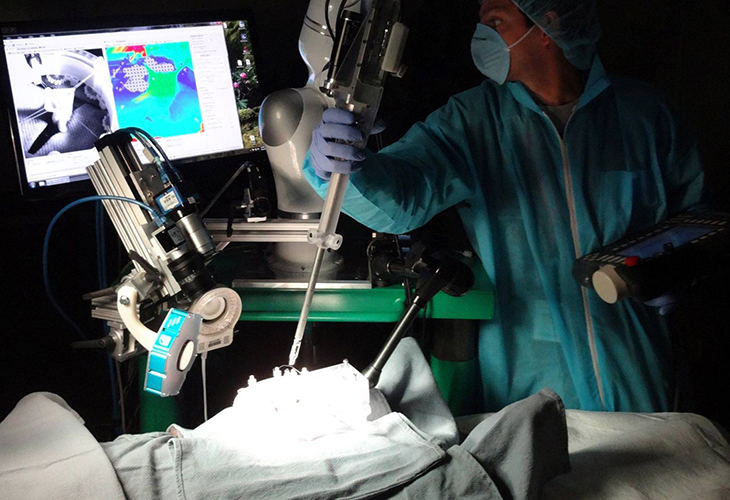
The STAR robot autonomously produced stitches that were more evenly spaced than those done by a surgeon, which is a good indicator of a suture’s strength.
3. Increased Dexterity and Precision
Robots' precision compared to humans has conferred advantages to a number of industries. This holds true for robotic surgical systems, and it can reduce surgical errors due to fatigue and imprecise wound closures.
Repetitive tasks in surgery, like suturing, are good candidates for robotic instruments because the tasks can be broken down into simple, easily defined movements. Procedures that require greater dexterity, like intestinal anastomosis or heart valve repair, are also good candidates for robotic automation because a robot can be designed with greater rotational freedom than the human hand. These extra degrees of freedom can be achieved by designing and testing a variety of end-effectors, which MANTA engineers have successfully done.
This increased precision promises to reduce procedure time. It also expands the range of procedures that robots can perform. For instance, the first human trial of a robot performing “supermicrosurgery,” or surgery on 0.3-0.8mm vessels, is currently underway. While only a very small number of surgeons can perform it, if the trial is successful, robots will also be able to repair microvasculature with greater precision and speed.

MUSA, the microsurgical robot from Microsure, has been shown to be safe and effective in suturing blood vessels to reduce lymphadema.
New surgical robotics systems will be able to perform repetitive tasks with more precision and greater autonomy, freeing up surgeons to focus on more complex aspects of a procedure and make more informed surgical decisions. With the surgical robotics landscape rapidly evolving, companies will need to additionally differentiate along factors such as usability and user experience. In Part Two, we'll dive into how advancements in sensors, haptics, and ergonomics can improve surgeon's interactions with the robot, as well as patient outcomes.
How Will Your Robot Transform Surgery?
Our experienced team of researchers, designers, and engineers can help you create a standout user experience, elegant enclosures, and cutting-edge electro-mechanical solutions. Get started now.

vidalista black 80mg tablets
vidalista black 80mg tablets
finasteride reddit pictures
finasteride reddit pictures
semaglutide tabletten rybelsus
semaglutide tabletten rybelsus
rybelsus semaglutid tabletter
rybelsus semaglutid tabletter
semaglutid köpa online flashback
semaglutid köpa online flashback